Lexapro, the brand name for escitalopram, is a selective serotonin reuptake inhibitor (SSRI) commonly prescribed for major depressive disorder and generalized anxiety disorder. It is one of the most widely used antidepressants because of its relatively favorable side effect profile compared to older drugs like tricyclics or MAOIs. Clinical trials consistently show that Lexapro is effective in reducing both depressive symptoms and anxiety, making it a first-line therapy in many treatment guidelines.
Lexapro causes hair loss in some patients, a condition often referred to as escitalopram hair loss or Lexapro-induced alopecia. Although relatively rare, case reports and pharmacovigilance studies document a link between escitalopram and hair loss, usually presenting as telogen effluvium; where a larger-than-normal number of follicles shift into the resting phase, leading to diffuse shedding.
Lexapro hair loss describes diffuse or patchy shedding that develops during treatment with escitalopram. It is a type of medication-induced alopecia, often reversible after discontinuation or dose reduction.
The mechanism appears to involve serotonin-related disruption of the hair growth cycle, where altered neurotransmitter signaling triggers premature follicle rest. A case series published in the Journal of Clinical Psychopharmacology (2018) reported escitalopram-associated alopecia in multiple patients, most of whom improved after switching medications or lowering the dose.
Is Hair Loss from Lexapro Considered Iatrogenic?
Yes. Hair loss from Lexapro is considered iatrogenic, meaning it is a side effect directly caused by the medical treatment itself rather than an unrelated illness.
How Common Is Hair Loss in People Taking Lexapro?
Hair loss from Lexapro (escitalopram) is considered rare, but it has been documented in pharmacovigilance studies and case reports. Most patients taking Lexapro do not experience hair shedding, but when it occurs, it typically presents as telogen effluvium, where a higher percentage of follicles enter the resting phase prematurely.
In the FDA Adverse Event Reporting System (FAERS) database, alopecia accounts for less than 1% of reported Lexapro side effects, making it an uncommon complication. A review in the Journal of Clinical Psychopharmacology (2018) noted that while SSRIs overall trigger hair loss, bupropion and mood stabilizers like valproate or lamotrigine are more strongly associated compared to escitalopram.
A 2021 pharmacovigilance study in Annals of Pharmacotherapy analyzed antidepressant-induced alopecia and confirmed that escitalopram was among the least frequently implicated SSRIs and hair loss due to medication, though cases do exist.
Hair loss on Lexapro is uncommon, affecting fewer than 1 in 100 patients, but when it occurs, it is usually reversible and linked to dose sensitivity or individual metabolic response.
Why Is Hair Loss a Side Effect of Lexapro (Escitalopram)?
Hair loss is a side effect of Lexapro (escitalopram) because the drug disrupts the normal hair growth cycle in some patients, most often by triggering telogen effluvium, where follicles prematurely enter the resting phase.
This disruption is tied to serotonin’s role in follicle regulation and blood supply to the scalp. By altering serotonin pathways, Lexapro disturbs the growth environment of follicles, leading to shedding in some patients. While rare, these cases of lexapro side effects hair loss have been reported in pharmacovigilance studies and case reports, and they often reverse once the dose is lowered or the medication is switched.
Does Escitalopram Make Your Hair Fall Out?
Yes. Escitalopram (Lexapro) makes your hair fall out, although it is an uncommon side effect. The condition, often described as escitalopram hair loss, usually presents as telogen effluvium, where a larger number of follicles enter the resting phase and shed prematurely.
Escitalopram and hair loss are linked, with several patients experiencing diffuse thinning during treatment. In most cases, hair regrowth begins within 3–6 months after dose adjustment or discontinuation according to “Hair Loss Associated with Escitalopram but Not with Venlafaxine” (Prim Care Companion CNS Disorders).
How Does Lexapro Cause Hair Loss?
Lexapro (escitalopram) causes hair loss by pushing follicles into telogen effluvium, where more hairs than usual enter the resting/shedding phase due to serotonin-pathway modulation and stress-hormone (HPA-axis/cortisol) responses that disrupt normal follicle cycling.
Escitalopram alters scalp microvasculature and keratinocyte activity, reducing growth signals and triggering diffuse shedding in susceptible patients. Evidence includes a case report of escitalopram-associated alopecia with regrowth after discontinuation ( Hair Loss Associated with Escitalopram but Not with Venlafaxine, Prim Care Companion CNS Disorders, 2011) and a report showing alopecia resolving after switching from escitalopram to duloxetine ( Alleviation of Alopecia after Switching from Escitalopram to Duloxetine, Düşünen Adam, 2016). Mechanistically, stress-related cortisol surges are known to impair follicle cycling and keratinocyte function, supporting this pathway ( Psychological Stress and Hair Loss: Possible Mechanisms, Experimental Dermatology, 2017).
How long does it take for Escitalopram to Cause Hair Loss?
Most cases begin after 2–3 months of therapy; one case started in the third month and resolved after stopping escitalopram.
How Does Lexapro Trigger Premature Entry into the Telogen Phase?
Lexapro (escitalopram) triggers premature entry into the telogen phase by altering serotonin signaling and stress-hormone regulation, which shortens the hair’s active growth (anagen) phase and accelerates shedding. This mechanism aligns with telogen effluvium, where a higher percentage of follicles than normal shift into the resting phase at once, leading to noticeable thinning across the scalp.
Pharmacologically, SSRIs like escitalopram influence the hypothalamic-pituitary-adrenal (HPA) axis and cortisol release, creating a stress-like state at the follicle level. Elevated cortisol disrupts dermal papilla cell activity, impairs microcirculation, and makes follicles more likely to miniaturize.
A documented case of escitalopram-induced telogen effluvium was published in Prim Care Companion CNS Disorders (2011), where hair shedding began three months after starting treatment and improved after discontinuation. This demonstrates how medication-induced follicular stress accelerates entry into telogen, producing diffuse hair loss.
What Distinguishes Anagen Effluvium from Telogen Effluvium in SSRI Users?
Anagen effluvium in SSRI users is marked by abrupt and severe hair loss that occurs when the drug interferes with actively growing hair follicles (anagen phase), leading to breakage or premature shedding of shafts. This is less common with SSRIs like escitalopram, but when it happens, hair loss is usually rapid and diffuse, resembling the effects of chemotherapy-induced alopecia.
Telogen effluvium is the more common hair loss pattern seen with SSRIs, where stress from medication, serotonin modulation, or cortisol imbalance pushes a disproportionate number of follicles into the resting (telogen) phase at once. This results in diffuse thinning that typically appears 2–3 months after starting treatment and improves once the drug is discontinued or adjusted.
A study in the Journal of Clinical Psychopharmacology (2015) reported that most SSRI-associated alopecia cases were telogen effluvium, while true anagen effluvium remained rare, highlighting the distinct mechanisms and clinical timelines of both conditions.
How Can Lexapro Disrupt Normal Hair Cycle Homeostasis?
Lexapro (escitalopram) can disrupt normal hair cycle homeostasis by altering serotonin signaling and hormone regulation, which indirectly affects the hair follicle’s growth cycle.
Serotonin and cortisol imbalances linked to SSRI therapy shift follicles from the active growth phase (anagen) into the resting phase (telogen), resulting in diffuse shedding. This disruption is not due to direct follicle toxicity but rather to systemic changes in neuroendocrine balance and stress-response pathways that control blood flow, nutrient delivery, and follicle cycling.
Drug-induced telogen effluvium is often tied to medications like SSRIs, where altered neurohormonal signals accelerate premature entry into the telogen phase, causing shedding within weeks to months of treatment, according to “Drug-Induced Hair Loss: Review of the Literature” (International Journal of Trichology, 2013).
How Does Neurotransmitter Dysregulation Influence Hair Follicle Function?
Neurotransmitter dysregulation impairs hair follicle function by disrupting signaling pathways that control follicle growth, cycling, and cellular metabolism. For example, serotonin (5-HT) directly activates dermal papilla cells and promotes gene expression tied to hair growth, so when serotonin signaling is altered (such as by SSRIs), this support to follicles weakens according to “Serotonin activates dermal papilla cells and promotes hair growth” published in PubMed.
Additionally, dopamine has been shown to trigger the catagen (regression) phase in human scalp hair follicles in vitro, indicating that shifts in neurotransmitter balance prematurely pushes follicles out of their growth phase.
Neurotransmitter imbalances alter the biochemical environment around hair follicles, disturbing normal cues for when to grow, rest, or regress; and thereby contributing to drug-induced hair loss vulnerability.
Does Lexapro Alter Dopamine or Norepinephrine in Ways that Affect Hair?
Yes. While Lexapro (escitalopram) is a selective serotonin reuptake inhibitor (SSRI) that primarily targets serotonin, it indirectly alters dopamine and norepinephrine pathways, both of which influence hair follicle health. By enhancing serotonin signaling, downstream effects suppress dopamine release in certain brain regions and modulate norepinephrine tone, leading to hormonal and stress-axis changes that affect hair cycling.
These shifts contribute to telogen effluvium, where follicles prematurely enter the resting phase. Serotonergic medications cause secondary alterations in catecholamine activity, which influence peripheral systems like hair follicles.
How Does Lexapro Cause Hair Loss in People with Depression?
Lexapro contributes to hair loss in people with depression by triggering telogen effluvium, where more follicles than usual abruptly shift into the resting phase, leading to diffuse shedding. This effect often overlaps with antidepressant hair loss observed in patients on SSRIs, and the impact is magnified in depressed patients who already have increased cortisol, inflammation, or nutritional deficiencies stressing the hair follicles.
A patient developed scalp hair loss due to depression around the third month of escitalopram use, which resolved after discontinuation according to “Hair Loss Associated with Escitalopram but Not With Venlafaxine” (Prim Care Companion CNS Disord, 2011).
Why Does Lexapro Cause Hair Thinning in Depressed Patients?
Lexapro causes hair thinning in depressed patients because the drug interferes with nutrient absorption and hormonal balance, weakening follicle structure and accelerating shedding. By altering serotonin pathways, escitalopram disrupts endocrine signals that regulate scalp vasculature, growth factors, and micronutrient transport; especially in individuals already vulnerable from depression. A patient developed diffuse hair loss while on escitalopram, which reversed after discontinuation in a case study called “Hair Loss Associated With Escitalopram but Not With Venlafaxine” (Prim Care Companion CNS Disord, 2011), highlighting this drug’s potential to impact follicle health.
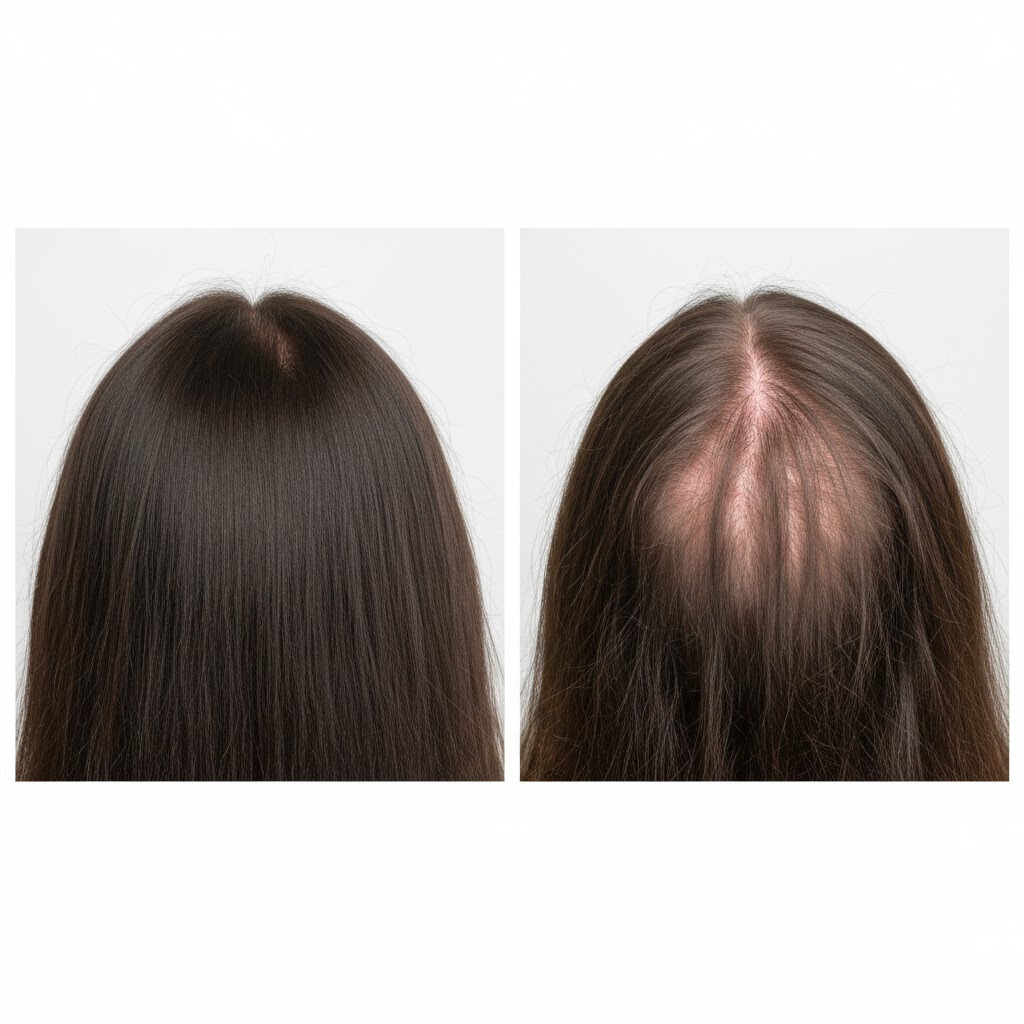
What Does Hair Look Like Before and After Lexapro Hair Loss?
Before Lexapro-related hair loss, patients typically maintain normal hair density and scalp coverage, but during treatment some develop diffuse thinning, reduced volume, and visible widening of the part line due to telogen effluvium. After dose adjustment or discontinuation, regrowth often begins within 3–6 months if follicles remain intact, though recovery varies depending on individual sensitivity and nutritional status.
How to Stop Hair Loss from Lexapro
Hair loss from Lexapro (escitalopram) is often managed or reduced with a combination of medical adjustments, lifestyle support, and targeted hair treatments. Recovery usually begins within 3–6 months if follicles remain intact, but success depends on individual sensitivity and treatment consistency.
- Medication Review: If hair shedding begins after starting Lexapro, a doctor adjusts the dose or switch to another SSRI with a lower risk of alopecia. Clinical case reports note regrowth within months after discontinuation.
- Nutritional Support: Ensure adequate intake of iron, zinc, vitamin D, and B vitamins, which are frequently linked to antidepressant-related shedding. Supplementation supports follicle recovery and improves regrowth success.
- Topical Treatments: Minoxidil (2%–5%) stimulates follicles during telogen effluvium episodes. It typically requires at least 3–4 months of consistent use for visible improvement.
- Stress and Hormonal Regulation: Since antidepressant hair loss is often tied to stress responses, stress-reduction practices and maintaining hormonal balance through medical supervision improve follicle resilience.
- Scalp Health Optimization: Regular use of gentle, sulfate-free shampoos and anti-inflammatory scalp treatments reduce irritation triggered by Lexapro and support follicle recovery. Research in the Journal of Dermatological Treatment (2020) shows that maintaining scalp pH balance helps restore hair density in patients with medication-related telogen effluvium.
How Effective Is a Hair Transplant for Lexapro-Related Permanent Hair Loss?
Hair transplant surgery is an effective solution for permanent hair loss caused by Lexapro (escitalopram), particularly in cases where medication-induced shedding stabilizes but follicles do not recover on their own. Since most Lexapro-related hair loss occurs through telogen effluvium and is reversible, transplantation is usually only recommended when thinning persists beyond 12–18 months despite discontinuation, nutritional support, or medical management.
When follicles are irreversibly miniaturized, a transplant restores density by relocating resistant grafts from the donor area to affected scalp regions. High graft survival rates are shown (90–95%) when performed under optimal surgical conditions, making transplantation a viable long-term option for drug-induced alopecia. (Hair Transplantation, 2024, StatPearls)
In Turkey, patients benefit from lower costs, advanced microsurgical techniques, and internationally accredited clinics. Among them, Vera Clinic is recognized as the best hair transplant clinic in Turkey, known for combining medical expertise, natural-looking design, and innovative methods that ensure consistent survival rates and high patient satisfaction.
What to Expect before and after a Hair Transplant for Lexapro Hair Loss?
Before the Transplant: Your surgeon confirms Lexapro-related shedding has stabilized, plans graft counts and hairline design, and preps donor/recipient sites for natural density.
After the Transplant: Expect brief redness and shedding by weeks 2–4, early regrowth from months 3–4, and fuller coverage by months 9–12 as grafts enter anagen.
Check the hair transplant before and after results caused by lexapro hair loss!
When to See a Dermatologist for Hair Loss due to Lexapro
You should see a dermatologist if Lexapro hair loss becomes severe, with rapid diffuse shedding, bald patches, scalp redness, or signs of infection that persist despite basic care. These symptoms indicate that the shedding is not just temporary telogen effluvium but could be aggravated by nutritional issues, hormonal changes, or drug sensitivity.
Early consultation is crucial to prevent progression to permanent thinning and to discuss recovery strategies, including whether a hair transplant consultation is appropriate if follicles show no regrowth after 12–18 months.
How is Lexapro Hair Loss Diagnosed?
Lexapro hair loss is usually diagnosed through medical history, scalp examination, and ruling out other causes such as thyroid disease or iron deficiency.
Which Other Type of SSRI Antidepressants Can Cause Hair Loss?
SSRI hair loss usually appears as telogen effluvium, where hair follicles prematurely shift into the resting phase. This differs from depression-related hair shedding, which is more tied to cortisol and stress hormones, because SSRI-induced hair loss begins after the medication starts and often improves after dose adjustment or discontinuation.
- Fluoxetine (Prozac): Fluoxetine can trigger SSRI hair loss through telogen effluvium, which is drug-induced and distinct from depression-related shedding.
- Wellbutrin (Bupropion): Although not an SSRI, Wellbutrin hair loss risk is higher than most SSRIs and differs from stress-related loss in depression.
- Paroxetine: Paroxetine causes reversible telogen effluvium, showing a medication effect separate from depression-driven hair thinning.
- Citalopram (Celexa): Citalopram hair loss often appears months after starting treatment, unlike depression hair loss which stems from cortisol imbalance.
- Sertraline: Sertraline can lead to temporary hair shedding as a side effect, differing from the gradual loss caused by mood-related stress hormones.
- Fluvoxamine: Fluvoxamine hair loss is rare but documented, and is directly drug-linked rather than the result of depressive illness itself.
Fluoxetine
Reports of fluoxetine and hair loss show a dose-related telogen effluvium pattern. Patients developed diffuse thinning that resolved after the drug was stopped. This confirms the distinction between medication-induced fluoxetine hair loss and depression-driven shedding.
Wellbutrin (Bupropion)
Although not an SSRI, wellbutrin hair loss is well-documented. Large cohort data show it has a higher risk of alopecia compared with SSRIs. Many patients improve after switching from bupropion to an SSRI. Here, the drug (not the depressive illness) drives the loss.
Paroxetine
Case reports highlight paroxetine hair loss confirmed by withdrawal-and-rechallenge testing: shedding stopped when paroxetine was discontinued and restarted when reintroduced. This shows medication causality rather than depression itself.
Citalopram (Celexa)
Patients on citalopram hair loss have reported diffuse thinning, often referenced as celexa hair loss. Symptoms of citalopram and hair loss usually started after several months and reversed once the drug was switched.
Sertraline
Several case series describe sertraline hair loss beginning within weeks of therapy. The diffuse shedding resolved when the dose was reduced or the drug discontinued, showing a direct drug effect.
Fluvoxamine (Prozac)
Though rarer, prozac and hair loss has been reported. Similar to other SSRIs, the fluvoxamine hair loss pattern is telogen effluvium, with recovery occurring once the medication was adjusted or replaced. This further supports that the effect is pharmacological rather than psychiatric.
Does Switching Antidepressants Reduce the Risk of Drug-Induced Alopecia?
Yes, switching antidepressants reduces the risk of drug-induced alopecia, but success depends on the individual drug and patient profile. Case reports show that patients experiencing hair loss on one SSRI (like escitalopram or paroxetine) often improved after transitioning to alternatives with lower reported incidence, such as fluoxetine or sertraline. However, the risk is not completely eliminated, as hair loss recurs with other agents in the same drug class.
Regrowth typically began within 3–6 months after discontinuation or switching according to “Antidepressant-Induced Alopecia: A Review of Case Reports” (Journal of Clinical Psychopharmacology, 2018), highlighting the importance of close monitoring and dermatological consultation when adjusting therapy.