A hair transplant involves relocating healthy hair follicles from the donor area to regions affected by thinning or baldness. For most patients, the best donor area is the back and sides of the scalp. This region is genetically resistant to the hormone DHT (dihydrotestosterone), which is responsible for most cases of male and female pattern baldness. Because these follicles are naturally more durable, they continue to grow for a lifetime once transplanted to areas affected by thinning.
During the procedure these follicular units are generally extracted using the Follicular Unit Extraction (FUE). The key is to harvest only as much as needed, maintaining the donor site’s density and aesthetic appearance. Once the grafts are removed, the donor area enters its recovery phase and tiny extraction points (in FUE) begin to heal. With proper post-operative care, redness and scabbing fade within weeks, and within a few months, the area blends naturally with the rest of the scalp.
The donor area is more than just a “source” for grafts; it’s the foundation on which a successful hair transplant is built. Preserving its health ensures both the longevity of the transplanted hair and the natural look of the remaining hair. In skilled hands, it remains a silent partner in the transformation, hidden, yet essential.
Where Are the Donor Areas for Hair Transplants Located?
When planning a hair transplant, understanding the hair transplant donor area is crucial; it determines the quality, density, and longevity of the transplanted hair. While every patient’s scalp anatomy is unique, surgeons typically target regions where hair is naturally resistant to hair loss.
- Occipital Scalp (Back of the Head):The most common good donor area for hair transplant procedures is the occipital scalp; the zone stretching across the back of the head, just above the neck. Hair in this area is genetically programmed to resist the effects of dihydrotestosterone (DHT), the hormone responsible for follicular miniaturization in androgenetic alopecia. Because of this resistance, grafts taken from here tend to grow for a lifetime, even when transplanted to thinning areas.
- Parietal Zones (Sides of the Head): The sides of the scalp, also DHT-resistant, are another reliable hair transplant donor site. These areas often serve as a secondary source of grafts when the occipital region does not provide enough follicular units to meet the patient’s goals. Side donor areas also tend to blend well cosmetically after extraction, making post-surgery healing less noticeable.
- Permanent vs. Non-Permanent Donor Zones: A permanent donor zone refers to areas where hair retains its growth cycle and thickness throughout life, even in patients with advanced hair loss. By contrast, non-permanent donor zones, such as the upper sides or crown, are susceptible to thinning over time. Transplanting hair from non-permanent zones lead to unpredictable results, as those grafts eventually miniaturize and shed.
Weak donor areas are typically found in the crown, upper temples, or regions already showing early signs of thinning. Grafts from these zones are less reliable for long-term survival and are generally avoided by skilled surgeons.
Why Is the Occipital Scalp Considered the Best Donor Area?
The occipital scalp refers to the back portion of the head, stretching from just above the nape of the neck to the upper rear of the skull. It is widely recognized as the gold standard donor site in hair transplantation because of its follicular stability, genetic resistance to hair loss, and consistently high hair density compared to other regions of the scalp.
The occipital region typically contains one of the highest follicular unit densities on the scalp, averaging 65 – 85 follicular units per cm², depending on the patient’s ethnicity and genetics. These follicles also tend to remain stable over a lifetime, making them a dependable source for long-term hair restoration. Anatomically, this area lies within what surgeons call the permanent hair zone, a band of hair that is minimally affected by progressive baldness patterns.
One of the primary reasons the occipital scalp is considered the best donor area is its resistance to dihydrotestosterone (DHT), the androgen hormone that causes follicular miniaturization in androgenetic alopecia. Occipital follicles have fewer androgen receptors, making them less responsive to DHT and therefore much less likely to thin over time as indicated in the article ‘Androgenetic alopecia: An update’, Sincengile Ntshingila et al. (2023), published in the Journal of the American Academy of Dermatology.
Compared to other potential donor areas, hair from the occipital scalp is often thicker in diameter, darker in pigment, and more robust. These qualities contribute to better coverage and a more natural appearance after transplantation. The strength of these follicles also increases their survival rate during the extraction, handling, and implantation stages.
Some patients, particularly those with extensive hair loss or depleted scalp donor areas, require supplemental sources such as beard hair or body hair as stated in “Body Hair Transplant by Follicular Unit Extraction: My Experience With 122 Patients”, Sanusi Umar, (2016). Beard hair, in particular, is often coarse and resilient, making it suitable for adding density, though it differs in texture from scalp hair and is typically used for mid-scalp or crown coverage rather than the hairline.
What Are the Different Zones of the Donor Area in a Hair Transplant?
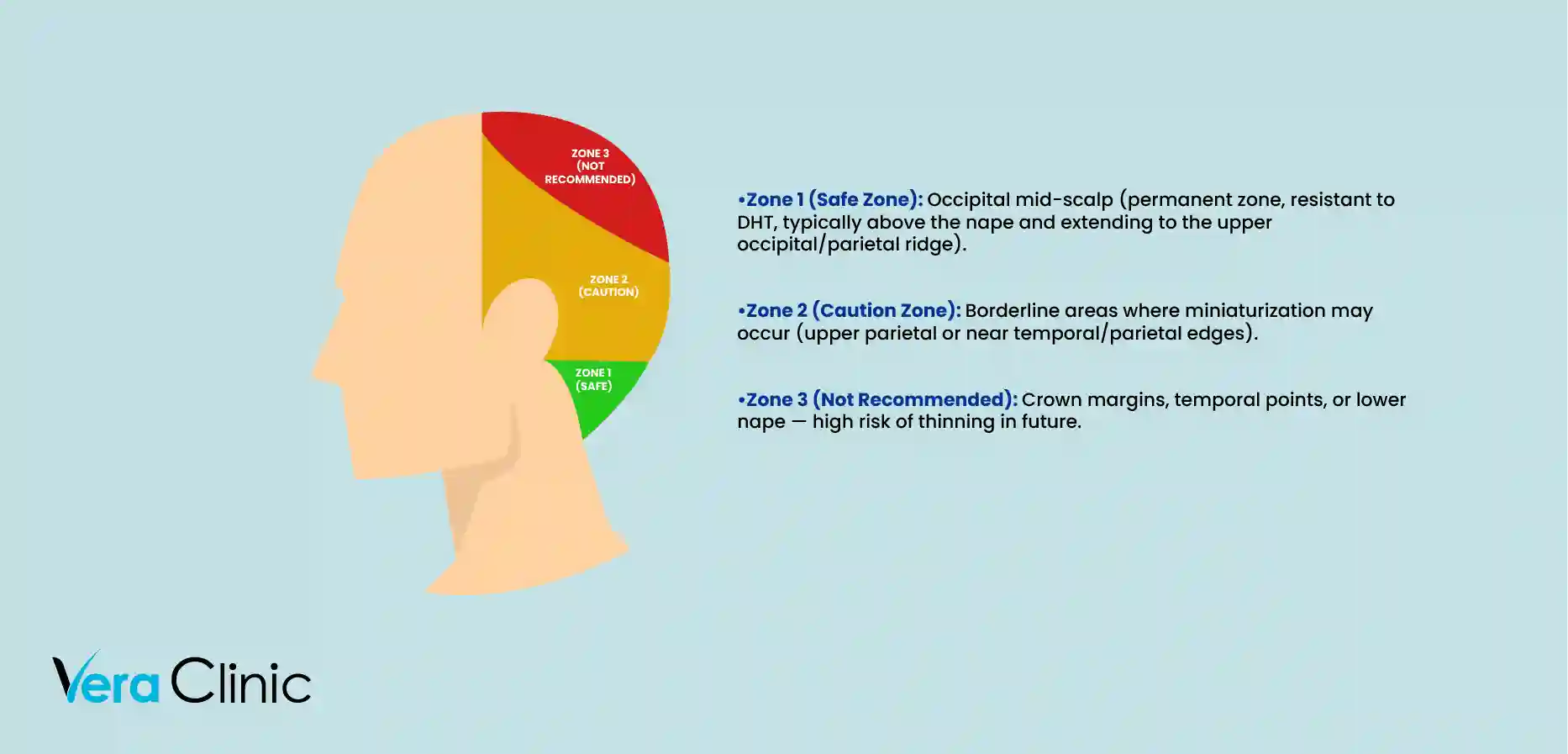
In hair restoration, the donor area is divided into specific zones based on long-term follicular stability and susceptibility to hair loss. Understanding these hair transplant zones helps surgeons extract grafts strategically, ensuring the transplanted hair remains permanent while preserving the natural density of the donor site.
- Permanent Donor Zone (Zone 7 Donor / Zone 5 Donor): The permanent donor zone, sometimes referred to in surgical mapping as Zone 7 or Zone 5 depending on the classification system, includes the mid-occipital scalp and extends horizontally along the back of the head to the mid-parietal areas above the ears. Follicles here are genetically resistant to DHT (dihydrotestosterone), the hormone responsible for androgenic alopecia, making them the most reliable for long-term survival.
- Borderline Donor Zone (Zone 4 Donor / Zone 3 Donor): This area sits just above or outside the permanent donor zone, including the upper occipital region, lower temporal areas, and scalp above the ears. While these follicles are still relatively stable in early to moderate hair loss cases, they thin over time, especially in patients with advanced male pattern baldness. Harvesting heavily from Zone 4 donor or Zone 3 donor regions carries a risk of future graft loss if those hairs eventually miniaturize.
- Non-Permanent Donor Zone (Zone 2 Donor and Beyond): These zones include the crown (vertex), frontal hairline areas, and high temporal points. They are the least stable, highly susceptible to thinning, and generally not recommended for graft extraction. Any hair transplanted from these regions follow the same progressive loss pattern as the original hair in those zones.
Extracting outside the safe donor zone increases the risk of transplant failure over time, as grafts from unstable regions eventually thin or disappear. Skilled surgeons use clinical experience, microscopic assessment, and patient hair loss history to map these zones accurately, ensuring only genetically stable follicles are transplanted.
Why Is the Safe Donor Zone Crucial for Successful Hair Transplants?
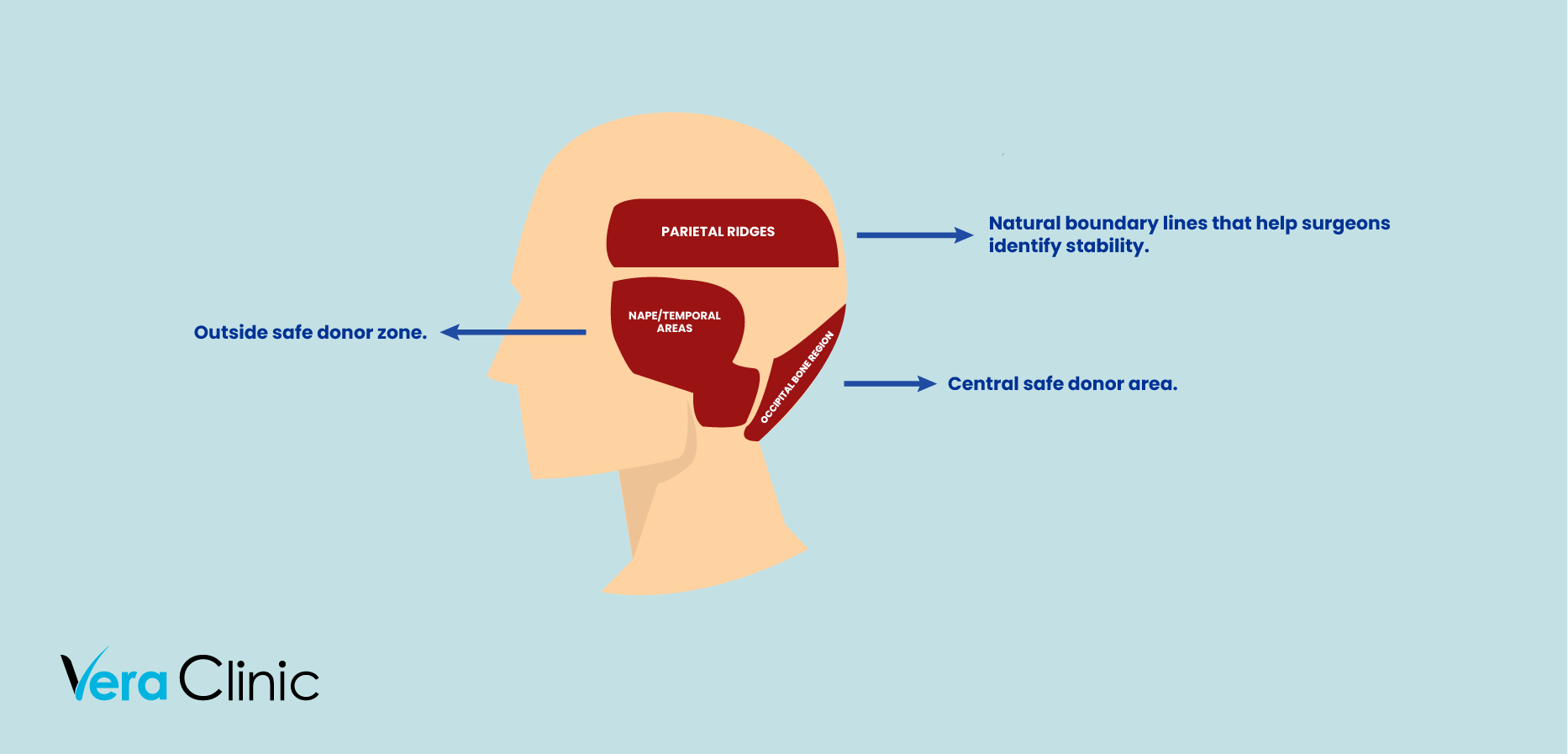
The safe donor zone, also known as the Norwood safe zone, is the band of hair at the back and sides of the scalp that remains largely unaffected by androgenetic alopecia, or pattern hair loss. It typically spans the mid-occipital scalp and extends into the mid-parietal areas above the ears. This region has been identified through decades of clinical observation as containing follicles that maintain their growth for a lifetime, even in individuals with advanced stages of baldness.
Surgeons define its boundaries using the Norwood scale: the upper limit sits just below the parietal ridge where the top of the head curves into the sides. The lower limit lies just above the nape of the neck, and the lateral limits fall midway above the ears, avoiding the higher temporal areas that are prone to thinning over time. Staying within these boundaries ensures that graft extraction is confined to permanent hair zones, reducing the risk of future loss as indicated in the article “Assessment of Safe Donor Zone of Scalp and Beard for Follicular Unit Extraction in Indian Men, A Study of 580 Cases”, Chouhan et al., (2019).
Extracting grafts from areas outside the safe zone significantly increases the risk of long-term transplant failure. While hair from borderline or non-permanent zones look healthy during surgery, it is often genetically predisposed to thin in later years. When such grafts are transplanted, they miniaturize and shed over time, resulting in patchy or uneven coverage as stated in the article “Hair Transplantation: Basic Overview”, Jimenez et al., Journal of the American Academy of Dermatology (2021).
The occipital and mid-parietal regions within the safe zone offer distinct anatomical and genetic advantages, including fewer androgen receptors, which makes them less susceptible to the effects of dihydrotestosterone (DHT); the hormone that causes follicle shrinkage in pattern baldness.
How Does Donor Dominance Influence the Success of Hair Transplant?
Donor dominance is a foundational principle in hair transplantation: transplanted follicles retain the genetic and biological traits of their original location regardless of the recipient site. In other words, hair extracted from a genetically resistant donor area continues to thrive and grow, even when relocated to areas prone to thinning.
This principle was first articulated in the 1950s by Dr. Norman Orentreich, the pioneer of modern hair restoration. He observed that transplanted hair from the back and sides of the scalp continued to grow permanently, even when placed in bald, androgen‑sensitive zones, thus establishing the concept of donor dominance. His findings were foundational, laying the groundwork for modern transplantation techniques.
Supporting this, hair transplantation is rooted in the principle of donor dominance, where transplanted hair retains its genetic identity and growth fate, determined by the donor, not the recipient site as affirmed in the study, “Hair Transplantation”, Orentreich, D. S., et al., (1985), published in the Journal of Dermatologic Surgery and Oncology.
Autografts maintain their characteristics after transplantation, irrespective of the new location according to the academic literature “Autografts in Alopecias and other selected dermatological conditions”, Orentreich, N. (2006). Additionally, when follicles are extracted from the occipital scalp, their inherent growth behavior and immunity to adverse conditions persist post-transplant in the recipient area as indicated in the article, “Follicular Unit Extraction [FUE]: One Procedure, Many Uses”, Kerure et al., (2020).
These clinical observations underscore why donor site quality outweighs the recipient site’s condition. Harvesting hair from the occipital region, known for its permanence and DHT resistance, means transplanted follicles continue to grow robustly in recipient areas. Conversely, if follicles from less stable, thinning regions are used, they fail long-term, even under optimal surgical technique.
How Many Grafts Can Be Safely Extracted from the Donor Area?
The number of grafts that are safely extracted from the donor area over a patient’s lifetime depends on several anatomical and surgical factors. On average, most individuals have a lifetime donor supply of around 4,000 to 6,000 grafts, though this figure varies based on natural hair density, hair characteristics, and extraction technique. Each graft generally contains 1 – 4 hairs, translating to 8,000 to 15,000 hairs in total.
Safe extraction limits are determined by factors such as follicular density, hair shaft caliber, scalp laxity, age, and hair loss progression. For example, patients with higher natural follicular density or thicker hair shafts achieve better coverage with fewer grafts. Scalp flexibility also plays a role; more elastic scalps allow for easier harvesting, particularly with FUT, whereas tighter scalps require a more conservative approach. The surgical method matters too; FUT yields more grafts in a single procedure without excessive thinning, while FUE spreads the extractions across a broader area to minimize visible depletion.
Surgeons must also plan with the future in mind. Overharvesting causes donor depletion, leaving the back and sides of the scalp visibly thin or patchy. This risk increases if more than 20 – 25% of the donor density is removed in one session, particularly with FUE. Since donor follicles do not regenerate, long-term preservation is essential.
Clinical research supports these guidelines. Patients safely yield 4,000 – 6,000 lifetime grafts, while removing less than 15% of donor follicles in a single pass helps preserve density according to the article “Another Way to Look at Donor Harvesting Effects with FUE”, Paul T. Rose (2016) published in the ISHRS-Hair Transplant Forum International. The same article advises surgeons to anticipate future hair loss patterns and harvest conservatively to avoid visible thinning as patients age.
In short, the safe extraction limit is not a fixed number, but a careful calculation unique to each patient. A skilled surgeon weighs current goals against long-term donor preservation, ensuring that today’s results do not compromise tomorrow’s options.
What Happens to the Donor Area After a Hair Transplant?
After a hair transplant, the donor area, usually the back and sides of the scalp, begins a predictable healing process that varies slightly depending on the extraction method (FUE or FUT) and the patient’s individual healing capacity.
In the first few days, it is normal to see small red dots (in FUE) or a linear incision (in FUT) where grafts were removed. Mild swelling, tenderness, and scabbing occur, but these generally start subsiding within the first week. Proper aftercare, such as gentle cleansing and avoiding scratching, helps prevent irritation or infection.
By around the donor area after 10 days, most scabs have fallen off, redness has significantly reduced, and any discomfort has usually resolved. In FUE procedures, tiny extraction points begin to close and blend with the surrounding hair. In FUT cases, the incision line is healing, and it is possible to have the sutures or staples (if used) removed during this time.
Over the following weeks, hair in the donor area continues to grow normally. Temporary “shock loss” (telogen effluvium) occurs in surrounding hair due to surgical trauma, but this is usually temporary and regrows within a few months.
Proper harvesting within the safe donor zone leads to high healing rates, minimal scarring, and preservation of follicular density over time as evidenced in the study “Donor Harvesting: Follicular Unit Excision”, Anil K Garg et al., (2018). With experienced surgical technique and conservative harvesting, the donor area maintains its natural density and appearance long-term.
How to Tell If Your Donor Area Is Damaged After Hair Transplant
A damaged donor area refers to the part of the scalp, typically the back and sides, that has sustained excessive trauma, scarring, or thinning after a hair transplant. This damage often occurs when the safe donor zone is not respected, when overharvesting in a hair transplant removes too many follicles, or when poor surgical techniques lead to unnecessary injury and slow healing. The main causes include unskilled extraction methods, exceeding safe graft limits, harvesting from non-permanent areas, and post-operative complications such as infection or inadequate wound care as indicated in the study “The donor area”, Russell G. Knudsen, MB, BS. (2004).
Signs of a damaged donor area include patchy or uneven density that gives a “moth-eaten” appearance, wide or multiple scars (in FUT) or large visible white dots (in FUE), persistent redness or raised skin due to poor healing, and noticeable thinning compared to the original density as evidenced, “Follicular Unit Extraction for Hair Transplantation: An Update”, Jiménez-Acosta et al., (2017).
Preventing donor area damage starts with selecting an experienced, board-certified hair transplant surgeon with a proven track record in donor management. It is essential to keep harvesting within the safe donor zone, follow all post-operative care instructions to avoid infection, and ensure that graft removal is kept within safe density limits. Large sessions should be planned strategically, sometimes combining FUT and FUE to preserve density.
If damage has occurred, several treatment options are available. Scalp micropigmentation (SMP) creates the illusion of density by tattooing small pigment dots to mimic hair follicles. Corrective hair transplant surgery redistributes remaining donor hair to improve evenness. Platelet-rich plasma (PRP) therapy promotes healing and stimulates weak follicles, while certain laser treatments help remodel scar tissue and improve skin texture.
Donor area depletion is among the most preventable complications in hair restoration and is usually linked to overharvesting hair transplant or poor technique as stated in the research “Complications in Hair-Restoration Surgery”, Konior, R. J. (2013).
Aggressive FUE extraction without considering long-term hair loss patterns is the leading cause of visibility of a damaged donor area. This is especially seen in patients with low density or advanced hair loss as indicated in the study “Determining Safe Excision Limits in FUE: Factors That Affect, and a Simple Way to Maintain Aesthetic Donor Density”, Sharon A. Keene et al., (2018) published by the International Society of Hair Restoration Surgery (ISHRS).
Does the Hair Transplant Donor Area Regrow After Extraction?
No. Once hair follicles are removed from the donor area during a hair transplant, they do not grow back. This is because the follicle itself is the living structure responsible for hair production, and when it is fully extracted, that growth site is permanently gone. The concept is similar to transplanting a plant root; once it is moved, the original spot no longer produces growth.
However, the appearance of the donor area after extraction still looks full if the procedure is performed skillfully. Factors that help maintain a natural look include precise surgical spacing (avoiding the removal of adjacent follicles), high hair caliber (thicker hair shafts provide more visual coverage), and good native hair density (more surrounding hairs help conceal extraction points). For example, in Follicular Unit Extraction (FUE), surgeons typically leave small gaps between harvested grafts to allow existing hair to camouflage the tiny wounds as they heal.
In the first week, small red dots (FUE) or a linear incision (in FUT) are visible. By 10 – 14 days, scabs usually fall away, and surrounding hair begins to grow longer, making the extraction points less noticeable. Over time, as the hair in the donor zone continues its normal growth cycle, the area appears unchanged to the casual observer, but this is purely an optical effect, not true regrowth.
The principle of donor dominance ensures transplanted follicles grow in their new location, but hair transplant donor area regrowth does not occur according to the article “Follicular Unit Hair Transplantation: Current Technique”, Jiménez-Acosta et al., (2009). Preservation of the donor zone’s appearance relies entirely on careful harvesting and respecting safe extraction limits.
Is Severe Pain in the Donor Area After Hair Transplant Normal?
No, severe or persistent pain in the donor area after a hair transplant is not considered normal and should be evaluated by your surgeon. Some mild to moderate discomfort is expected in the first few days following surgery, especially in Follicular Unit Transplantation (FUT) where a linear incision is made, or in Follicular Unit Extraction (FUE) where multiple small punches are used. This normal post-surgical discomfort typically feels like soreness, tightness, or tenderness and usually improves significantly within 3 – 5 days, with most patients reporting minimal or no pain by the end of the first week.
However, severe pain in donor area after hair transplant, especially if it worsens instead of improving, indicates a complication. Possible causes include infection, hematoma (blood collection under the skin), nerve irritation, or excessive swelling. Infections also present with redness, heat, and discharge, while nerve irritation causes burning or shooting sensations. Overharvesting or overly aggressive extraction also contributes to hair transplant pain after the procedure, sometimes accompanied by prolonged sensitivity or numbness.
If the pain is intense, persists beyond the first week, is accompanied by fever, swelling, or pus-like discharge, or is progressively worsening, it’s important to contact your surgeon promptly.
What Causes Scarring in the Hair Transplant Donor Area?
Scarring in the donor area is an expected outcome of a hair transplant, but its type and visibility depend on the technique used and the patient’s healing process. In Follicular Unit Transplantation (FUT), a strip of scalp is removed from the back of the head, leaving a hair transplant back of the head scar in the form of a fine line. When closed with a trichophytic method, it is concealed under hair about 1-2 cm long, with the FUT scar healing timeline showing redness fading in weeks and the hair transplant scar maturing over several months. In Follicular Unit Extraction (FUE), multiple small punches leave tiny circular marks known as FUE donor area scars, which are often less visible but become more noticeable if overharvesting occurs.
Scar visibility is influenced by the surgeon’s skill, scalp elasticity, hair and skin characteristics, and natural healing ability. While no procedure leaves the donor site completely scar-free, various methods camouflage scars after hair transplant. These include trichophytic closure during FUT, scalp micropigmentation (SMP) to replicate hair follicles, and even transplanting hair into scar tissue for better blending.
Most patients find that donor scars are easily hidden with modest hair length, but those keeping very short styles still notice either a faint linear scar or a series of pale microdots. Choosing an experienced surgeon, following post-operative care instructions, and having realistic expectations are key to achieving the best aesthetic outcome.
Does the Donor Area Leave Scars After a Beard Transplant?
Yes, a beard transplant leaves small, permanent scars in the donor area, although these are usually minimal and often go unnoticed once healing is complete. In most procedures, the donor hair is taken from the scalp and extracted using the Follicular Unit Extraction (FUE) method. This creates tiny circular wounds that heal over time, leaving microdot scars. In some cases, donor hair is also taken from under the chin or jawline, and the same principle applies: each extracted follicle leaves a small mark once healed.
The visibility of these scars depends on several factors, including the surgeon’s technique, the patient’s beard donor area healing response, skin tone, hair density, and how well post-operative care instructions are followed. In most healthy patients, a beard transplant heals rapidly and the surrounding hair conceals the marks effectively as indicated in the article “Beard transplantation”, Carlos Eduardo Guimarães (2017), Brazilian Journal of Plastic Surgery.
With skilled extraction and good aftercare, the beard transplant donor area typically heals well, and any residual scarring is only visible upon close inspection or if the hair is shaved extremely short. For patients concerned about scar visibility, techniques such as scalp micropigmentation (SMP) or strategic hair length maintenance further conceals the donor sites.
Why Does Shock Loss Affect the Donor Area After Hair Transplant?
Shock loss refers to the temporary shedding of existing, non-transplanted hair in or around the surgical area following a hair transplant. In the donor area, this phenomenon occurs when the trauma from follicular unit extraction (FUE) or strip removal (FUT) temporarily disrupts the hair growth cycle. The native hairs surrounding the extraction points enter the telogen phase (resting phase), leading to shedding in the weeks after surgery.
Shock loss in the donor region is temporary or permanent. Temporary shock loss is far more common, the follicles remain intact, and new growth resumes within 3–6 months. Permanent shock loss is rare and generally happens if the surrounding hair was already miniaturizing due to androgenetic alopecia; in such cases, surgical trauma accelerates its natural loss.
The main causes of donor shock loss are surgical trauma to nearby follicles and temporary disruption of blood supply during the extraction process as claimed in the article “Donor Area Acute Effluvium following Follicular Unit Extraction – Trichoscopic Simulator of Alopecia Areata: Series of Four Cases”, Amit S Kerure et al., (2020). Additional factors like overharvesting, aggressive punch sizes in FUE, or tension on the wound edges in FUT increase the risk.
Most patients recover fully without intervention. To minimize the risk of a hair transplant shock loss, experienced surgeons maintain conservative extraction patterns, avoid excessive tension on tissues, and ensure proper wound care. Preventive measures also include pre-operative finasteride or minoxidil (in patients without contraindications) to strengthen existing hair before surgery.
Donor shock loss is a recognized but usually self-limiting effect of hair transplantation, resolving as the follicles naturally re-enter the growth phase as indicated in the article “Complications in Hair Transplantation”, Amit S Kerure et al., (2018), published in the Journal of Cutaneous and Aesthetic Surgery. For patient reassurance, it’s important to emphasize that this is part of the normal healing cycle and does not indicate permanent damage to the donor area.
Which Hair Transplant Techniques Affect the Donor Area?
Different hair transplant techniques impact the donor area in unique ways, influencing its appearance, scarring, healing process, and recovery timeline. In Follicular Unit Transplantation (FUT), a strip of scalp is surgically removed from the back of the head, and follicles are dissected from it for transplantation. This method leaves a single linear scar that is usually concealed with hair as short as 1–2 cm, provided a skilled surgeon performs a trichophytic closure. Healing time is generally a few weeks for discomfort and redness to subside, but scar maturation takes several months.
Follicular Unit Extraction (FUE), including advanced hair transplant techniques like Direct Hair Implantation (DHI) and Robotic FUE, involves extracting individual follicular units directly from the scalp using small punches. This creates multiple tiny circular wounds across the donor zone, known as FUE donor area scars. When performed with precision and proper spacing, these scars are barely visible, especially if the hair is kept at a short length. Recovery is often quicker than FUT, with most patients returning to normal activities within days, and full healing typically occurring within 1–2 weeks. However, aggressive or uneven harvesting leads to visible patchiness and donor depletion.
DHI is a variation of FUE in which the extracted grafts are immediately implanted using a Choi implanter pen. This reduces graft handling time and improves survival rates, but the donor area impact remains similar to conventional FUE since the extraction process is the same. Robotic FUE uses image-guided precision to optimize punch depth and angle, potentially reducing tissue trauma and improving donor healing outcomes, though results still depend heavily on the surgeon’s expertise.
The pros and cons vary. FUT offers more grafts in a single session and preserves surrounding donor density but leaves a noticeable linear scar. FUE provides minimal visible scarring and faster recovery but requires meticulous technique to avoid overharvesting. DHI and Robotic FUE add precision and implantation efficiency, but their advantages are only fully realized in experienced hands. Surgeon skill, safe donor zone management, and conservative harvesting have a greater influence on donor appearance and long-term results than the choice of technique alone as specified in the article “Complications in Hair Restoration Surgery”, Raymond J. Konior, (2013).
What Happens During Hair Transplant Donor Area Recovery?
Hair transplant donor area recovery follows a predictable healing process, with some variations depending on whether the procedure was performed using Follicular Unit Transplantation (FUT) or Follicular Unit Extraction (FUE). Immediately after surgery, the donor area appears red and swollen, with small crusts or scabs forming over extraction points in FUE, or along the linear incision in FUT. Mild tenderness or tightness is normal and typically improves within the first few days.
Week 1-2 marks the most visible healing phase. In FUE, tiny dot wounds begin to close, scabs naturally fall off, and redness gradually fades. In FUT, the incision line starts to heal and sutures or staples (if used) are usually removed within 7 to14 days. During this time, patients generally resume gentle hair washing using the clinic’s recommended method, but they should avoid scratching, rubbing, or high-pressure showering directly on the donor area.
By Week 3-4, most patients notice that the donor area blends well with the surrounding hair, especially if they maintain a slightly longer hairstyle. Any lingering pinkness in fair-skinned patients continues to fade. Physical activities such as light exercise are resumed after the first week, but heavy lifting, swimming, and contact sports should be postponed for at least 2-3 weeks to protect the healing tissue.
Between Month 2 and Month 6, the donor zone continues to mature. In FUT cases, the linear scar softens and becomes less noticeable, following a FUT scar healing timeline that extends up to 12 months for complete scar remodeling. In FUE, the small extraction dots typically become almost invisible, although very short haircuts reveal them.
With proper surgical technique and aftercare, hair transplant recovery time for the donor area is relatively short, and permanent aesthetic changes are minimal when extractions are performed within safe limits as stated in the article “Hair Transplantation”, Jennifer Goldin (2025).
Following the surgeon’s post-operative instructions, including sleeping position, wound cleaning, and activity restrictions, plays a crucial role in achieving optimal hair transplant donor area recovery and long-term preservation of density.
What to Expect in the Donor Area 1 Month After a Hair Transplant
At one month post-surgery, the donor area is usually well into the healing phase, with most early post-operative symptoms resolved. In both FUT and FUE, the initial redness and swelling have typically subsided, and any scabs or crusts from extraction points are fully healed. Patients notice a faint pink tone in lighter skin types or mild residual pigmentation in darker skin, but this gradually blends with the surrounding scalp color over time.
For a FUE donor area after 1 month, the tiny circular extraction sites are closed and no longer tender. Short stubble is usually visible as new hair growth begins in the donor zone, although shock loss, temporary shedding of native hair around the extraction sites, and make the area appear slightly thinner. In FUT cases, the linear scar is in its early maturation stage; while the incision line is sealed, the surrounding skin still feels tight, and numbness in a small area above or below the scar is possible but typically improves in the following months.
Some patients still experience mild itching, tingling, or tightness in the donor area at this stage, but these sensations are part of normal nerve recovery and usually continue to improve. Gentle hair washing, styling, and even light trimming are generally safe by the one-month mark, although chemical treatments or aggressive scalp manipulation are best postponed until at least 8–12 weeks post-op.
By 4 weeks, donor site healing is largely complete at the surface level, but deeper tissue remodeling continues for several months. Proper post-operative care, including following washing protocols, avoiding sunburn, and not scratching the healing skin, supports optimal cosmetic recovery for both the donor area after 1 month and long-term density preservation as stated in the article, “Complications in Hair Transplantation”, Amit S Kerure et al., (2018), Journal of Cutaneous and Aesthetic Surgery.
Why Does the Donor Area Feel Itchy After Hair Transplant?
Itching in the donor area after a hair transplant is a normal part of the wound-healing process. When tiny incisions (in FUE) or a linear strip removal (in FUT) begin to heal, the skin’s nerve endings regenerate and new tissue forms, triggering signals that the brain interprets as itchiness. This sensation is also caused by increased blood flow and the release of histamines as part of the body’s inflammatory response to surgery.
Nerve regeneration plays a significant role in this phase. During follicle extraction, some superficial nerve endings in the skin are temporarily disrupted. As they reconnect and heal, patients often experience tingling, prickling, or itching sensations. Skin repair also contributes, as the epidermis and dermis remodel, small scabs fall away and collagen is produced, which creates tightness and itch.
Itching usually peaks during the first 7 – 14 days after surgery and gradually lessens as healing progresses. For most patients, it is mild and short-lived, but in some cases, low-grade itchiness persists for several weeks while deeper tissues continue to recover.
Safe ways to relieve itching include using surgeon-recommended saline sprays, applying mild post-op moisturizers, or taking prescribed antihistamines to calm the histamine response as mentioned in the study “Complications in Hair Transplantation”, Amit S Kerure et al., (2018). It’s important to avoid scratching or rubbing, as this disturbs healing tissue and increases the risk of infection or scarring. It is important to avoid scratching or rubbing, as this disturbs healing tissue and increases the risk of infection or scarring.
While hair transplant itching is usually harmless, there are situations where it could indicate a problem. If the itching becomes intense, is accompanied by redness, swelling, heat, discharge, or worsening pain, it is a sign of infection or folliculitis and should be checked by the surgeon immediately.
Post-operative itch is a common and self-limiting symptom of hair restoration surgery, linked to normal nerve regeneration and skin healing. Proper aftercare, hydration, and patience are usually all that’s needed for it to resolve naturally as indicated in the article “Self-management in the post-hair transplantation recovery period among patients with androgenetic alopecia: A qualitative study”, Liu Shichang et al., (2024).
How Long Does Full Healing After Hair Transplant Take?
Full healing after a hair transplant involves two distinct processes, recovery of the donor area and the growth of hair in the recipient area, each following its own timeline. In the donor area, superficial healing typically takes around 10–14 days. By this stage, the scabs have shed, the redness has faded, and the skin surface is closed. For patients who undergo Follicular Unit Extraction (FUE), the small circular extraction sites generally blend with the surrounding hair within two to three weeks. In Follicular Unit Transplantation (FUT), the incision line also seals within a similar timeframe, though deeper tissue healing, scar maturation, and nerve regeneration continues for three to six months depending on factors such as scalp elasticity, age, and aftercare quality.
In the recipient area, growth follows a slower cycle. After the procedure, transplanted follicles enter a resting phase, with visible shedding, known as shock loss, typically occurring within the first 2 to 4 weeks. New hair growth usually begins around the 3 to 4-month mark. Cosmetic improvement becomes more noticeable between six and nine months, and the hair continues to thicken, darken, and improve in texture until approximately 12 to 18 months after surgery, when the final result is fully visible.
For a typical FUE donor area recovery timeline, the first 1 to 3 days are marked by redness, mild swelling, and scabbing. Between days 4 and 7, the scabs begin to shed naturally and redness fades. By 10 to 14 days, the extraction points are closed and most patients have a normal appearance. In weeks 3 to 4, any remaining pinkness subsides and early hair regrowth starts to conceal the area. By 3 to 6 months, the tissue is fully healed, blending seamlessly with the surrounding hair.
These timelines vary from person to person, influenced by age, skin type, surgical method, and adherence to post-operative instructions. The best outcomes are achieved when donor harvesting is performed precisely, the safe donor zone is respected, and patients follow proper aftercare routines as explained in the article “Effect of Follicular Unit Extraction on the Donor Area”, Muhamamd H. Mohmand, et al., (2018).
How Long Does It Take for the Donor Area to Recover After FUE?
In most cases, the FUE donor area recovers remarkably quickly at the surface level, though complete healing and full cosmetic blending take longer. Within the first few days, it is possible for patients to notice mild redness, pinpoint scabs, and slight tenderness where follicles were extracted. By around 7–10 days, these scabs naturally fall away, and redness significantly fades. At two weeks, the FUE donor area after 2 weeks is typically well-healed on the surface, with only faint marks visible if the hair is shaved very short. Most patients resume normal grooming, light exercise, and daily routines by this stage without risk to the healing sites.
Deeper healing, including restoration of skin tone, nerve regeneration, and scar maturation, continues over several months. By 3 to 6 months, the donor zone usually blends seamlessly with the surrounding hair, and any minor textural changes are barely noticeable. For the majority of patients, the FUE recovery time of a FUE hair transplant for full visual integration is complete within this period. However, it’s important to note that the 1 year FUE donor area often looks its absolute best, at this point, both the extraction sites and the surrounding native hair have gone through multiple growth cycles, achieving optimal density and texture.
In terms of hair coverage, the donor area does not experience true follicular regrowth because extracted follicles do not regenerate (FUE donor area regrowth refers instead to the recovery of surrounding hair that has shed due to temporary shock loss). This regrowth typically begins at 2 to 3 months and restores the appearance of density, even though the exact number of follicles is reduced.
Several factors delay or disrupt recovery. These include overharvesting (removing too many grafts from a concentrated area), aggressive punch techniques, infection, poor post-operative care, smoking, and certain medical conditions that impair healing. Patients who follow their surgeon’s aftercare instructions, including gentle washing, avoiding scratching, protecting the scalp from sunburn, and spacing high-intensity activities, tend to achieve faster, more complete healing.
When performed within safe donor zone limits and with proper extraction patterns, FUE leaves minimal visible scarring and maintains the donor area’s natural appearance over the long term, as indicated in the article, “Determining Safe Excision Limits in FUE: Factors That Affect, and a Simple Way to Maintain Aesthetic Donor Density”, Sharon A. Keene et al., (2018). Skilled surgical technique combined with responsible patient care is the best predictor of a donor area that looks healthy both weeks and years after the procedure.
Which Factors Affect Healing in the FUT Donor Area?
Healing in the FUT donor area depends on several factors, including surgical technique, scalp characteristics, and patient aftercare. The FUT hair transplant timeline shows that surface healing usually takes 2 to 3 weeks, while deeper tissue and scar maturation continue for several months.
The FUT scar healing timeline is strongly influenced by surgeon skill. Techniques like trichophytic closure help create finer scars by allowing hair to grow through the incision. Patients with good scalp elasticity usually heal with narrower scars, while tighter scalps stretch the wound and make scars wider. Individual healing ability also plays a role, with age, skin type, and a tendency to form hypertrophic or keloid scars affecting results.
Other factors include hair and skin contrast, darker, thicker hair provides better coverage, while straight, fine hair reveals scars more easily. Lifestyle choices, such as smoking or poor wound care, delay healing and make scars of a FUT hair transplant more visible. Following post-operative instructions carefully helps minimize complications and ensures smoother recovery.
What Are the Signs of Healthy Healing After Hair Transplant?
During the recovery process, it is important to know what normal healing looks like so patients are able to distinguish it from possible complications. Healthy healing signs are generally consistent across both donor and recipient areas, although the exact pace varies between individuals.
- Reduced Redness: Mild redness is normal in both the donor and recipient areas during the first week. By 10–14 days, the redness should gradually fade without spreading or worsening. Persistent redness with pain suggests irritation or infection.
- Scabs Falling Off Naturally: Small scabs form around grafts or extraction points within the first few days. Healthy healing is seen when these scabs start to shed on their own after 7–10 days. Forcing them off too early damage grafts or slow healing.
- Absence of Excess Swelling: Some swelling around the forehead or donor zone appear in the first 3–4 days, but it should improve quickly. Swelling that worsens or spreads unusually is a red flag.
- No Pus or Unusual Discharge: A healthy healing process does not include pus, foul odor, or excessive discharge. Clear fluid or mild crusting is expected early on, but yellow or green discharge signals infection.
- Mild Itching or Tingling: Itching is a common sign of skin and nerve regeneration. It should be mild and improve within two weeks. Severe itching with pain or rashes point to an allergic reaction or folliculitis.
- Gradual Symptom Relief: Tenderness, tightness, or numbness in the donor area usually decreases week by week. If symptoms worsen or persist beyond the normal hair transplant recovery time, medical evaluation is recommended.
How Can Patients Support Healing After a Hair Transplant Donor Procedure?
Supporting donor area recovery requires consistent aftercare and lifestyle adjustments. Patients who follow medical guidance and maintain healthy habits experience faster recovery and fewer complications compared to those who neglect aftercare as indicated in the study “Follicular Unit Extraction Hair Transplant”, Aman Dua et al., (2010).
- Use the clinic’s recommended shampoo and technique, starting after the surgeon’s approval (usually 48 to 72 hours). Wash with lukewarm water, avoid high-pressure showering, and gently pat the area dry to prevent disturbing healing grafts.
- Protect the donor area from direct sun exposure for at least four weeks. Ultraviolet rays darken scars, irritate sensitive skin, and slow the healing process. A loose-fitting hat or scarf is safe once the donor area is sealed.
- Refrain from smoking and alcohol for at least one to two weeks post-surgery. Both reduce blood circulation and oxygen delivery to the scalp, which delays wound healing and increases the risk of poor scar quality.
- Support recovery with a nutrient-rich diet. Adequate protein helps tissue repair, vitamin C aids collagen production, zinc supports wound closure, and biotin strengthens new hair. Staying well-hydrated is equally important for skin repair.
- Avoid heavy exercise, contact sports, sweating, and wearing helmets for two to three weeks. Excessive friction, pressure, or sweat irritate the donor zone and delay healing. Light walking is usually safe after the first few days.
- Adhere to wound care, medication, and follow-up schedules for proper recovery and to minimize risks of infection or scarring.
Donor area scarring, healing, and patient satisfaction in 30 cases was studied and it was found that trichophytic closure produced more cosmetically acceptable scars, especially when strip width was minimized, according to the research “A Study of Donor Area in Follicular Unit Hair Transplantation”, Balakrishnan Nirma et al., (2013).
How to Prevent Donor Area Infection After Hair Transplant
Infection in the donor area after a hair transplant is rare, but following proper hygiene and aftercare steps is essential to ensure safe healing and prevent complications.
- Keep the area clean. Wash the donor site only as instructed by your surgeon, usually starting 48 to 72 hours after surgery. Use mild, recommended shampoo and lukewarm water, gently patting dry instead of rubbing.
- Avoid touching or scratching. Hands carry bacteria, so avoid scratching, rubbing, or picking scabs in the donor zone. Allow scabs to fall off naturally to protect healing tissues.
- Follow medication guidelines. Take all prescribed antibiotics, anti-inflammatory medication, or topical ointments as directed. These significantly reduce the risk of infection during the early healing phase.
- Protect from sun and dirt. Keep the donor area out of direct sunlight, dust, and pollution for at least 2 to 3 weeks. Sunburn or environmental contaminants irritate wounds and increase infection risk.
- Refrain from smoking and alcohol for at least 1 to 2 weeks. Both reduce blood circulation and weaken the immune response, slowing healing and increasing infection susceptibility.
- Avoid heavy exercise, sweating, or activities requiring helmets for 2 to 3 weeks. Excessive moisture and friction disrupt healing and introduce bacteria.
- Watch for persistent redness, warmth, swelling, pus, or worsening pain. These indicate infection and should be reported to your surgeon immediately for treatment.
- Follow the surgeon’s aftercare plan. Every patient receives personalized instructions. Adhering closely to these, from wound care to follow-up visits, is the most effective way to prevent complications.
How Can Donor Depletion Be Prevented After Hair Transplant?
Donor depletion refers to the permanent thinning, patchiness, or visible scarring in the donor area after hair transplant surgery, usually caused by excessive or uneven extraction of follicles. This compromises both the natural look of the donor site and the long-term sustainability of future procedures. Donor site management is one of the most critical factors in achieving lasting results according to the study “Hair Transplantation: Management of Donor Area”, Gerard E. Seery, (2002), Dermatologic Surgery.
- Recognize the aesthetic risks. Pay attention to how grafts are removed. Taking too many from one area can leave the donor zone looking “moth-eaten,” with visible scalp that’s difficult to conceal with shorter hairstyles.
- Calculate the safe extraction limit. Work within the patient’s lifetime graft capacity. On average, this is 4,000–6,000 grafts, but the exact number depends on density, hair caliber, and scalp elasticity.
- Maintain uniform spacing. Distribute extractions evenly across the donor zone. Avoid concentrating graft removal in one spot to preserve natural, balanced density.
- Avoid overharvesting. Never remove more than 20–25% of follicular units in one session. Plan long-term, especially for younger patients or those with progressive hair loss.
- Choose an experienced surgeon. Select a board-certified specialist who understands donor zone boundaries, anticipates future loss patterns, and applies precise extraction techniques to maintain density for life.